Abstract
Triazole resistant A. fumigatus has been documented in many parts of the world. In the Netherlands, incidence is now above 10% and results in the need for long-term parenteral therapy with liposomal amphotericin B (LAmB). The long terminal half-life of LAmB suggests that intermittent dosing could be effective, making the application of outpatient antifungal therapy (OPAT) possible. Here, we report our experience with the use of OPAT for Invasive Fungal Infections (IFI).
All adult patients treated with LAmB with a 2 or 3 times weekly administration via the outpatient departments in four academic tertiary care centers in the Netherlands and Belgium since January 2010 were included in our analysis. Patient characteristics were collected, as well as information about diagnostics, therapy dose and duration, toxicity, treatment history and outcome of the IFI.
Methods
Study setting and patient population
A multicenter retrospective cohort study was conducted within the Netherlands and Belgium. OPAT was applied at the home of the patient or within the hospital outpatient department. All adult patients treated with LAmB with a less frequent than daily administration via the outpatient departments of Leiden University Medical Center, Erasmus MC Rotterdam, Radboud University Medical Center Nijmegen, and the University Hospitals Leuven since January 2012 were included.
Study protocols and definitions
Typically for Aspergillus disease, a 3 mg/kg dose was started. For Mucor species a typical dose was between 5 and 10 mg/kg. The choice to start treating with intermittent therapy with LAmB was made according to the clinical judgment of the treating physician usually based on imaging and clinical course. Patients that were started on OPAT with LAmB were closely monitored for the occurrence of nephrotoxicity.
Analyses
Descriptive statistics of clinical variables of patients were calculated using the complete data set. Kaplan-Meier curves of survival during OPAT with LAmB were constructed. The analyses were performed using STATA v. 16 (Statacorp, College Station, TX, USA).
Ethics
The institutional review board from UZ/KU Leuven in Belgium approved the study. Data were processed after pseudonymization by the local investigators and in accordance with Personal Data Protection Acts of the respective countries.
Results
Between January 1st 2010 and September 1st 2018, a total of 18 adult patients received LAmB as an outpatient in a dosing frequency of 2 or 3 times a week. Triazole resistance, demonstrated by either polymerase chain reaction (PCR) or culture, has been the most common reason (in 10 cases) to choose treatment with LAmB instead of voriconazole in the patients with invasive aspergillosis.
Of all patients, nine (50%) were male, and the median age was 60 years. Fourteen patients (78%) had a hematological malignancy as underlying predisposing disease. A response to treatment prior to discharge and start of OPAT with LAmB was confirmed by CT scan in 17 patients. For the remaining patient, clinical improvement had been the reason to proceed with OPAT. Patients switched from daily treatment as an inpatient to intermittent OPAT with LAmB after a median of 56 days (range 14–193 days).
Median dosage of liposomal amphotericin B was 3 mg/kg, administered 3 times each week. Resolution of infection was finally achieved in 13 patients. The remaining patients were readmitted to the hospital, switched to another antifungal, died, or were lost to follow-up. Nephrotoxicity during OPAT occurred in 10 cases, of which in only one case treatment needed to be switched to another antifungal agent (posaconazole, after establishing intermediate sensitivity). Figure 1 shows the survival rates of all patients in a Kaplan Meier analysis since the start of OPAT.
 Figure 2 shows the time until resolution of infection.
Figure 2 shows the time until resolution of infection.
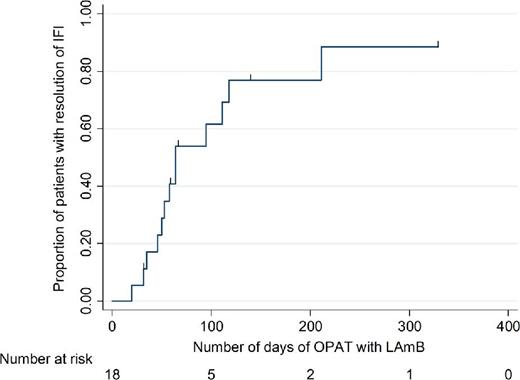
Figure 3 shows the time until nephrotoxicity occurred during intermittent treatment.
Discussion
This study shows that the use of OPAT with LAmB in a 2 or 3 times weekly dosing scheme results in high rates of therapy response in a selected patient population and after confirmation of an initial response to daily IV therapy with LAmB. The majority of patients in this study needed prolonged use of LAmB for the treatment of triazole resistant A. fumigatus infections.
In many cases, the clinician may fear the presence of resistance in case of worsening of clinical or diagnostic parameters after treatment with a triazole even with negative or absent resistance tests. Because of difficulty in establishing triazole-resistance or sensitivity, the clinical suspicion of resistance is becoming an important reason to abstain from further treatment with triazoles and opting for LAmB instead.
Nephrotoxicity has significantly decreased after the introduction of the liposomal formulation of amphotericin B. Application of OPAT strategies are slowly expanding within the field of infectious diseases and are being implemented in regular practice. Similar to LAmB, intravenous vancomycin therapy is also associated with renal toxicity but has nonetheless been successfully implemented in an OPAT program for many years now. Despite early reluctance, the expected logistic and toxicity-related disadvantages are outweighed by the advantages of a decrease in hospital stay with similar therapeutic effectiveness thanks to the implementation of monitoring of toxicity and therapeutic drug monitoring.
Source:
Robert J van de Peppel, Alexander Schauwvlieghe, Ruth Van Daele, Isabel Spriet, Jan W van’t Wout, Roger J Brüggemann, Bart J A Rijnders, Bart J C Hendriks, Mark G J de Boer. Medical Mycology, Volume 58, Issue 7, October 2020, Pages 874–880, https://doi.org/10.1093/mmy/myz134




