Abstract
Aspergillosis complicating severe influenza infection has been increasingly detected worldwide. Recently, coronavirus disease–associated pulmonary aspergillosis (CAPA) has been detected through rapid reports, primarily from centers in Europe. We provide a case series of CAPA, adding 20 cases to the literature, with review of pathophysiology, diagnosis, and outcomes.
The syndromes of pulmonary aspergillosis complicating severe viral infections are distinct from classic invasive aspergillosis, which is recognized most frequently in persons with neutropenia and in other immunocompromised persons. Combined with severe viral infection, aspergillosis comprises a constellation of airway-invasive and angio-invasive disease and results in risks associated with poor airway fungus clearance and killing, including virusor inflammation-associated epithelial damage, systemic immunosuppression, and underlying lung disease.
Radiologic abnormalities can vary, reflecting different pathologies. Prospective studies reporting poor outcomes in CAPA patients underscore the urgent need for strategies to improve diagnosis, prevention, and therapy.
Methods
Case Series
Cases of CAPA were identified during March–June 2020 at Johns Hopkins University and Hospital Clinic of Barcelona by review of microbiologic and infectious diseases consult data, with approval of the institutional review boards of both institutions.
Cases were defined as recovery of Aspergillus species from respiratory fluids (tracheobronchial secretions, sputum, bronchoalveolar lavage [BAL]) or positive (index ≥1) serum or BAL markers, identified with work-up for possible secondary pneumonia, typically clinically indicated with new fever or respiratory decompensation with new focal infiltrates on chest radiograph or computed tomography (CT) scan.
Results for a Fungitell β-d Glucan Assay were reported when available but did not suffice to establish case diagnosis; 60 pg/mL was considered intermediate and ≥80 pg/mL was considered positive. Neither center used PCR-based testing for fungal infections during this period.
Analyses
We calculated descriptive statistics for all data. These values are shown as frequencies, means (±SD), medians (with ranges), and proportions.
Results
Characteristics of Cases
Patient-level data were compiled in cases recognized before June 2020 at Johns Hopkins Medical Center and Hospital Clinic of Barcelona. Demographics mirrored those described for poor overall outcomes; advanced age and underlying diseases of hypertension and pulmonary disease predominated.
The most common immunosuppressing agents associated with CAPA included systemic or inhaled steroids, most frequently for adjunctive management of COVID-19 related inflammatory disease. CAPA was recognized a median of 11 days after symptom onset and 9 days after ICU admission.
Most of these patients were hospitalized during stages characterized by inflammation or acute respiratory distress syndrome or afterwards, with lung injury, in the ICU and required respiratory support.
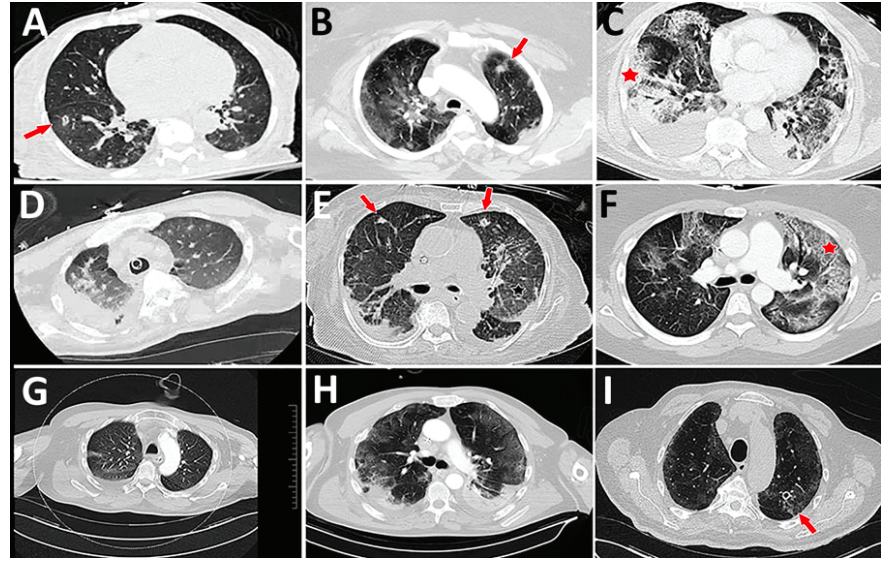
In cases for which CT scans were performed, radiographic reports generally described a mixture of findings attributable to the virus, findings consistent with airway inflammation and mucous, and radiographic findings consistent with airway-invasive disease (Figure 1).
Bronchoscopy was rare, and diagnosis was most frequently supported by tracheal aspirate culture; few patients had positive serum biomarkers. Seventeen (85%) cases were identified by positive culture; most (12/17, 71%) were identified by detection of A. fumigatus. Although rarely used, results of Fungitell β-d glucan assays were more frequently positive compared with serum galactomannan assays. All but 2 patients were given intravenous antifungal drugs, which included voriconazole, posaconazole, or liposomal amphotericin B.
One patient (#2) was not treated for findings of a nodule and positive serum galactomannan result, was extubated, and survived. Another patient (#12) had diagnosis of CAPA established 1 day before death and never received antifungal therapy
Synopsis of Literature
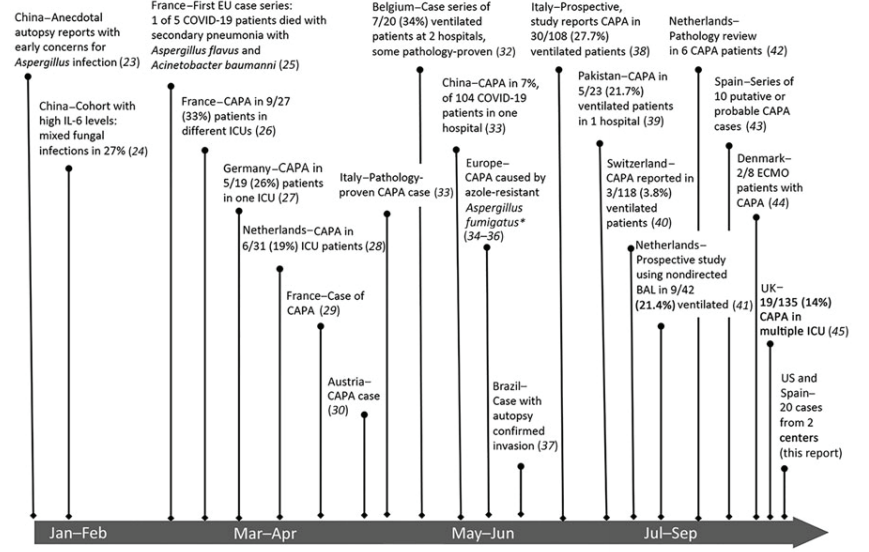
Evidence of secondary aspergillosis developing in persons infected with severe acute respiratory syndrome coronavirus 2 was first evident in China but emphasized more clearly by case series from Europe. We provide a timeline of studies describing secondary aspergillosis occurring in persons with COVID-19, an entity that has become referred to CAPA (Figure 2).
Figure 1. Representative computed tomography (CT) scans for 9 patients with aspergillosis complicating severe viral pneumonia in patients with coronavirus disease. The nodules and cavitating nodules are indicated by red arrows, and prominent airway thickening and bronchiectasis in ground glass opacities are indicated by red stars.
Patient-level descriptions emerged quickly in small case series from Europe. In the first case series from Europe for COVID-19, a total of 1 of 5 patients had alveolar infiltrates on chest radiograph and Aspergillus spp. cultured from tracheal aspirate. Thereafter, rapid reports from centers in Austria, Belgium, France, Germany, the Netherlands, and Italy emerged (Fig 2).
Differences in diagnostic methods and case definitions generated a wide degree of variability, and incidences ranged from 3.8% to 34% of persons admitted to ICUs. Higher mortality rates were noted for CAPA patients than for controls; there were trends to improved survival and decreased follow-up galactomannan levels after antifungal therapy.
Finally, another prospective study that used enhanced screening with blood and respiratory samples, antigen assays (galactomannan enzyme immunoassay [GM EIA] and β-d glucan assay), and an Aspergillus PCR reported that 19/135 patients met diagnostic criteria for CAPA when concurrent radiographic abnormalities were considered.
Discussion
Despite decades of case reporting and large cohort studies, many clinicians still fail to recognize that Aspergillus species can cause destructive inflammatory and invasive pathology in persons who have severe influenza, mistakenly ascribing culture results to benign airway colonization.
We add 20 cases to the accumulating literature describing CAPA. Multiple pathophysiologic, clinical, and diagnostic considerations have emerged from observations reported to date. These types of infections occur in persons who have more chronic immunosuppression, especially that related to prolonged steroids and chronic obstructive pulmonary disease.
Figure 2. Timeline of cases, series, and cohort studies reported to describe emergence of coronavirus disease–associated pulmonary aspergillosis. BAL, bronchioalveolar lavage; CAPA, coronavirus disease–associated pulmonary aspergillosis; ECMO, extracorporeal membrane oxygenation; EU, European Union; ICU, intensive care unit; IL-6, interleukin 6.
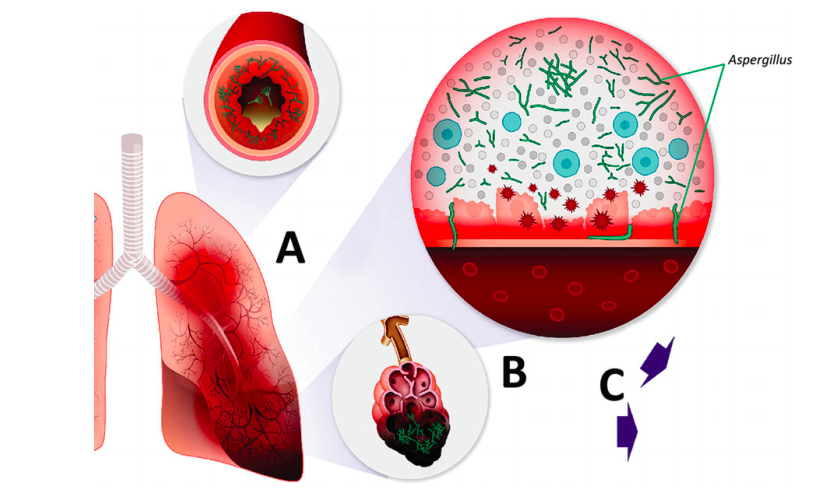
Mounting evidence suggests that severe respiratory virus infections, especially influenza and infection with severe acute respiratory syndrome coronavirus 2, can be complicated by Aspergillus airway overgrowth with pulmonary infection similarly characterized by mixed airway inflammation and bronchial invasion (Figure 3).
Performance of diagnostic testing is variable depending on immunopathogenesis of disease. Persons who have extensive invasion into and beyond airways show positive serum GM EIA results more frequently than persons who had disease restricted to the endobronchial lumen. For this reason, sensitivity of the serum GM EIA assay is highest in hematology/oncology patients, ranging from 60% to 80%, but lower in ICU patients, estimated to be 30%–50%.
In CAPA cases, serum GM EIAs have been infrequently positive. In our case series, results of β-d glucan assays were more frequently positive, but false-positive results would be anticipated because of to cross-reactivity. A study reported a relatively large proportion of cases with positive results for β-d glucan assays for patients who had candidiasis.
When applied to BAL, results for GM EIA appear positive more frequently, and some investigators reported potential utility of quantitative PCR or GM lateral flow tests in lavage. Despite diagnostic limitations, several studies point to utility in routine use of fungal biomarkers and early screening in persons who have COVID-19, especially directed toward BAL.
Radiographic manifestations might be best understood when one considers that CAPA can be a constellation of mixed airway and invasive diseases.
Conclusion
Although many questions linger, emerging evidence supports the conclusion that Aspergillus species cause mixed pathology in COVID-19 patients, ranging from airway inflammation to semi acute or acute bronchial invasion, similar to severe influenza infections. Increased efforts are needed to determine the best ways to prevent, diagnose, and treat Aspergillus disease associated with COVID-19.
Source: Marr KA, Platt A, Tornheim JA, Zhang SX, Datta K, Cardozo C, et al. Aspergillosis Complicating Severe Coronavirus Disease. Emerg Infect Dis. 2021;27(1):18-25. https://dx.doi.org/10.3201/eid2701.202896




